Undergraduate course information
Contacts and inquiries
UTS Student Centres
The UTS Student Centres are both the initial and primary point of contact for all students. Students should deal with the student centres in all matters affecting their studies. This includes enrolment, exemptions, timetable matters, examination and assessment, as well as a wide range of student administration procedures.
For specific Health information, students should contact the UTS Building 10 Student Centre. Opening hours vary during session.
Building 10 Student Centre
Foyer, Level 2, Building 10 (CB10.2)
235 Jones Street, Ultimo
telephone +61 2 9514 1222
Ask UTS
Clinical Practice Unit
Open from 9am till 4.30pm Mon-Fri (Phone and Counter) excluding public holidays.
The Clinical Practice Unit manages student placements by requesting and securing placements in over 100 health facilities and placing students in over 5500 individual clinical settings each year.
Students who have issues regarding their clinical placement or while they are on clinical should contact the unit on:
telephone +61 2 9514 5122
email health.clinical.practice@uts.edu.au
Laboratories technical officers
Laboratories technical officers maintain Health's laboratories and other student technical resources. Bookings for and queries about the laboratories and resources, as well as queries regarding safety issues, should be directed to:
telephone +61 2 9514 4916
Moore Park Precinct Sport and Exercise Science
Geoff Warman, Laboratory Services Manager
telephone +61 2 9514 5939
Faculty Academic Programs Office
The Academic Programs Office provides support and assistance to the UTS Student Centres on UTS: Health processes and issues and manages and supports Health's courses and specific student issues and processes. Students must contact the UTS Student Centre in the first instance and complex issues may be referred by staff in the UTS Student Centre to the Academic Programs Office.
Course Director
Course Directors provide academic advice to students on their program and other assistance such as helping students who experience difficulties coping with their academic work.
Bachelor of Nursing Course Director
Sonia Matiuk
CB10.07.201
telephone +61 2 9514 5717
Bachelor of Midwifery Course Director
Heike Roth
CB10.11.111
telephone + 61 2 9514 4806
Bachelor of Sport and Exercise Science/Management Course Director
Lee Wallace
MP01.03.026
telephone +61 2 9514 5333
Bachelor of Public Health Course Director
Albie Sharpe
CB10.08.114
telephone +61 2 9514 5236
Academic Liaison Officer
The Academic Liaison Officer (ALO) is responsible for assisting students with Special Needs negotiate, if necessary, reasonable adjustments to learning and assessment tasks with subject lecturers. Students with Special Needs include students who:
- have a disability or ongoing illness
- have significant primary carer responsibilities or are pregnant
Laura Sheridan
CB10.07.226
telephone +61 2 9514 5236
Associate Dean (Teaching and Learning)
The associate dean is responsible for the overseeing and quality of academic activities and the coursework programs.
Lynn Sinclair
CB10.06.153
Mobile Number +61 (0) 429 578 579
Faculty rules
Class allocation
Students are allocated to particular groups or classes within a subject. This class determines when they attend laboratory sessions as well as tutorial times. Students must state their preferences for classes at enrolment. Students are allocated to classes and may then make changes to their allocation (subject to available places). Further information on this process is available from My Subject Activities.
Some class changes may be limited by nursing practice restrictions in some years of the undergraduate courses, or by cohort management.
Nursing and Midwifery Board of Australia registration
The Bachelor of Nursing, Bachelor of Nursing Bachelor of Arts in International Studies, Bachelor of Midwifery and Bachelor of Midwifery Bachelor of Creative Intelligence and Innovation are accredited by the Nursing and Midwifery Board of Australia. Graduates are eligible to apply for registration as a Registered Nurse or Midwife. In addition, for registration eligibility, the Nursing and Midwifery Board of Australia requires applicants to provide evidence of identity and good character, and documented evidence for assessment of any variation to the standard education program, for example recognition of prior learning.
Clinical placements
UTS inherent requirements for nursing and midwifery undergraduate courses
Inherent requirements are the essential components of a course or subject that demonstrate the capabilities, knowledge and skills to achieve the core learning outcomes of the course. There are eight domains of inherent requirements in the nursing and midwifery undergraduate courses. Some domains have a number of sub-domains. These domains are:
- ethical behaviour
- behavioural stability
- legal
- communication
- cognition
- sensory ability
- strength and mobility
- sustainable performance.
It is a requirement of the nursing and midwifery undergraduate courses that students complete a number of clinical placements. Clinical placements are where a nursing or midwifery student goes out into the clinical setting to undertake the practical components of the course required for registration. If a student has a condition or disability that might prevent him or her from completing the placements, then completion of the degree may be delayed, or at worst, he or she may not be able to complete the degree. It is important that students read the full details about the inherent requirements for their course:
- Bachelor of Nursing (C10122)
- Bachelor of Nursing Bachelor of Arts in International Studies (C10123)
- Bachelor of Midwifery (C10225)
- Bachelor of Midwifery Bachelor of Creative Intelligence and Innovation (C10329)
Nursing practice policy
As part of their studies, students are required to undertake clinical practice in a variety of health facilities. This involves students being placed in a clinical environment in accordance with the nursing work integrated learning ladder. Students are provided with a clinical facilitator who supports their clinical learning and undertakes their assessment.
UTS: Health makes every effort to place students in a health facility in close proximity to their home or close to public transport. However, this is often very difficult to achieve given the limited number of student placements. Students should expect to travel across the greater Sydney region during their program to meet their clinical requirements. Reasonable adjustments can be made for students with special needs and/or carer commitments.
Carer commitment – where a student is the primary carer of an immediate family member/s; such requests must be supported by the faculty's academic liaison officer (ALO).
Special needs – where, for example, a student has a disability and/or an existing or ongoing illness; such requests must be supported by UTS: Accessibility Service.
Where a student has registered with either the ALO or UTS: Accessibility Services, reasonable adjustments are taken to accommodate them; however, this is still limited to available placements. Students are responsible for submitting a placement provisions form at the beginning of each sessionif they have clashing commitments, and need to consider the impact on their academic progression and ability to graduate on time. For more information, contact the Clinical Practice unit:
email health.clinical.practice@uts.edu.au
Midwifery practice policy
As part of their studies, students are required to undertake clinical practice. This involves students being placed in a midwifery practice environment in accordance with the midwifery work integrated learning ladder. Students are supported by a midwifery practice facilitator or midwifery educator. UTS: Health makes every effort to place students in a health facility in close proximity to their home and close to public transport. However, this is often very difficult to achieve given the limited number of student placements, and students are asked to take this into consideration when they receive notification of their placement.
Students with disabilities
Students in the Bachelor of Nursing, the Bachelor of Nursing Bachelor of Arts in International Studies, Bachelor of Midwifery or the Bachelor of Midwifery Bachelor of Creative Intelligence and Innovation must undertake nursing and/or midwifery practice placements as a prerequisite to satisfactory course completion. Information regarding the practice placement procedures for students with disabilities is available from Accessibility in the University-wide general information.
Students commencing this course must consider the inherent requirements to be able to achieve a passing grade in their clinical practice assessments. Students with concerns should contact UTS: Accessibility Services.
Accident and incident reporting
Any student or staff member involved in an accident, injury or incident while on clinical placement must complete a standard accident/incident form. Both the student and their supervising facilitator or educator are required to complete the form, in addition to any other form/s required by the facility.
If an injury sustained by a student raises doubts about the student's ability to attend subsequent nursing or midwifery practice experiences, the matter should be referred to the Manager, Clinical Liaison.
Attendance
The Nursing and Midwifery Board of Australia requires students to undertake a specified number of nursing or midwifery practice hours. One hundred per cent attendance on practice is required, excluding public holidays. Students who experience unforeseen illness or misadventure, as per UTS rule 8.3, are required to complete a special consideration application.
Students in this category may then be offered completion of nursing or midwifery practice at the next available relevant placement. Should a student fail to complete all nursing practice hours for any other reason, including work or social commitments, they will not be offered the opportunity to complete their nursing practice hours, and run the risk of failing the subject.
Students are required to attend designated shifts while on nursing practice. Shift times vary between facilities; however, common start times are 7am and 1.30pm.
Completion of nursing or midwifery practice
When assessing whether students are eligible to undertake additional hours to complete their nursing or midwifery practice, the Faculty of Health examines a student's nursing or midwifery practice history, taking into account past attendance as well as the requirements of the Nursing and Midwifery Board of Australia. Therefore, it is in the interests of students to ensure that they maintain a complete attendance record.
As indicated above, students may not be given the opportunity to complete missed nursing practice hours and consequently may fail the subject.
Conduct
Students undertaking supervised nursing or midwifery practice must follow the directions given to them by their facilitator, midwifery educator or academic liaison officer or, in the absence of these, the staff of the hospital or agency concerned. Students are reminded that they are required to adhere to clinical placement facility policy and procedures. While on clinical practice students are being assessed on their professional conduct and failure to adhere to facility policy and procedures including professional conduct may result in an unsatisfactory assessment.
Safety
While on practice placement, all students are responsible for promoting and maintaining environmental health and safety (EHS) by:
- looking out for hazards, reporting them to the supervisor of the work area and helping to fix hazards
- taking action to avoid, eliminate or minimise risks
- following safe work methods and using personal protective equipment as required
- seeking information or advice as necessary, particularly before carrying out new or unfamiliar work
- participating in orientation activities
- reporting accidents and incidents to the supervisor of the work area
- reporting emergencies in line with the facility protocols
- disposing of any hazardous wastes in a safe and approved manner
- not willfully placing at risk the health, safety and welfare of others
- exercising a duty of care toward others in everything undertaken.
All students must be aware of risk management policies and processes and be capable of implementing these within the clinical environments. Students must also comply with the policies and procedures of the relevant health facility.
Pregnancy on clinical placements
Pregnancy does not preclude students from clinical practice however some clinical placements may be potentially harmful to the developing foetus and to the student. Pregnant students are expected to notify the Faculty of Health of their pregnancy if they are working or studying in areas where there may be particular health and safety issues, e.g. radiation, working with infectious disease, cytotoxic drugs or anaesthetic gases.
If at any time a student's condition changes or they have been deemed to have a high-risk pregnancy, they must contact the Manager, Clinical Liaison for appropriate risk management and to determine the suitability of potential placements.
Students must also comply with health care facilities' guidelines and recommendations when undertaking placements. Where a student is pregnant it is recommended that they meet with the academic liaison officer (ALO) prior to census date to decide on the most appropriate course of action to ensure safety and progression concerns are addressed and planned for.
Student wellbeing advice
All students involved in clinical placements must be fit to do so.
Students who have health problems or who are under the influence of alcohol and/or other drugs that might foreseeably render them unsafe during nursing or midwifery practice placement, or who have a health problem that may be affected adversely during their placements, should seek medical advice before undertaking a placement and should advise the Manager, Clinical Liaison.
Failure to do so may result in the Faculty of Health accepting no responsibility for the consequences.
Each student is responsible for evaluating the foreseeable health risks before and during each clinical placement, and implementing risk management strategies in consultation with the subject coordinator, and UTS environmental, health and safety guidelines. Students must also adhere to policies and direction from workplaces where the clinical placement is held.
Uniform
Students are required to wear the official uniform of the Faculty of Health during all nursing and midwifery practice placements. Academic staff will indicate any other occasions when students must wear their uniform. Some nursing practice placements, e.g. mental health, may not require the official uniform. Students are notified of this when they receive their practice placements. Students must purchase their uniform from the approved suppliers.
The uniform consists of:
- purple polo shirt; UTS design (men and women)
- black trousers; (men and women)
- black knee-length skirt; (to be worn with stockings)
- black, closed in rubber-soled shoes.
Other requirements are as follows.
- Fingernails must be short and clean. Only clear nail varnish is acceptable.
- Artificial nails must not be worn by healthcare professionals providing patient care.
- Hair must be worn off collars. Students with long hair must wear it up; long ponytails are not acceptable.
- Students are permitted to wear a wedding ring and one pair of small, plain studs in the ear lobes. No other jewellery or piercings are acceptable.
- Watches should either be digital or have a second hand, and must have no sharp edges, fancy watchbands or large buckles. A multicoloured ballpoint pen and small notepad are essential requirements. A small pocket calculator is advisable.
- Academic staff will provide advice to students on other items which need to be purchased, e.g. fob watch, stethoscope, scissors.
- Students must wear the uniform from their first nursing or midwifery practice placement in Autumn session and should ensure that their uniform is available by this time.
- All students must wear their UTS photo identification card, with retractable cord, at all times near their collar; this is available from the Co-op Bookshop for a nominal fee.
Verification required to attend clinical
All nursing and midwifery students who are required to attend clinical practice as part of their program are required to meet the NSW Ministry of Health (NSW MoH) Verification requirements. These include, but are not limited to, complying with criminal clearances and the screening and vaccination against infectious diseases – evidence for the screening and vaccination against infectious diseases is recorded on a NSW Health Vaccination Record Card for Health Care Workers/Students which is available for collection at the CPU, UTS: Student Centres or UTS: Health Services. Meeting these requirements may result in costs to the student.
Please see NSW Health policies about vaccination:
- Occupation Assessment, Screening and Vaccination Against Specified Infectious Diseases
- Management of health care workers with a blood borne virus and those doing exposure prone procedures
Complying with these policies is now managed through the NSW MoH ClinConnect system and all students must be verified through this system to be attached to a placement. Students are recommended to commence collecting the information required when they are accepted into a Nursing or Midwifery course as students who are not verified are not able to be allocated placements.
UTS is committed to the health, welfare and safety of its students and staff. The following guidelines have been set up in order to ensure legislative requirements are adhered to, along with minimising infectious disease transmission to and/or from our students and staff.
All students and staff must adhere to current legislative requirements, policies and procedures regarding infection control and immunisation. Students should be aware of guidelines regarding immunisations and levels of required immunity, as indicated within these guidelines. At the time this policy was developed, guidelines assisting in the direction of this policy included:
- National Health and Medical Research Council (2003), The Australian Immunisation Handbook, 8th edn, Commonwealth of Australia, Canberra.
- NSW Health (2005a), Occupational Assessment, Screening and Vaccination Against Specified Infectious Diseases, Circ 2007/006, 1 February 2007.
- NSW Health (2005b), Tuberculosis Screening and Protection – Health Care Worker, Circ 2001/71, 1 August 2001.
Documentary evidence of vaccination and/or current immunity for the following diseases (completed record card plus serology) prior to clinical placement is mandatory:
- Adult Diptheria, Tetanus and Pertussis (dTpa vaccine)
- Hepatitis B
- Measles/Mumps/Rubella (MMR)
- Varicella (chickenpox)
- Tuberculosis
- Influenza (annual requirement).
Acceptable immunisation status is a prerequisite for attending clinical placements, due to legislative and organisational requirements. Health facilities have the right to preclude students who are not immunised in accordance with their policies. There are academic progress implications for students who fail to complete practice requirements for this reason.
Students who are unable to complete vaccination requirements for any reason (including conscientious objection) must request authorisation through the Manager, Clinical Liaison at least four weeks prior to every clinical placement. In most cases authorisation will be denied due to external organisation policies and requirements. Students who are unable to meet immunisation requirements will significantly impact their ability to complete their course.
Criminal record checks
Full details are provided in the NSW child protection legislation section in the University-wide general information.
First Aid course
All nursing students who are required to attend clinical practice as part of their program are required to complete an accredited First Aid Course by the end of session one of studies in the Bachelor of Nursing program/s.
Unsafe practice performance
A student's performance is deemed unsafe if it places patients, clients, their families, staff members or fellow students at risk, and if he or she is unable or unwilling to perceive that risk. The judgment that a student's performance is unsafe is usually made on the basis of more than one incident, however, it can be made on the basis of one episode.
Students whose performance is deemed unsafe are removed from the health facility as soon as the judgment is made and are referred to the Manager, Clinical Liaison, who determines the appropriate course of action. Students may receive a fail grade for the subject, or be given an opportunity to demonstrate improvement in an alternative clinical environment such as the laboratory. If satisfactory, students are given another opportunity to complete their nursing or midwifery practice in a clinical environment.
Refer to rule 16.10.
Unsatisfactory practice performance
A student's performance is deemed unsatisfactory if it fails to meet the objectives and assessment of a given nursing practice experience.
Each student has a formative assessment part-way through his or her clinical placement. If unsatisfactory performance is identified in this assessment, the clinical facilitator/midwifery educator/academic liaison officer notifies the student and identifies a plan of action. This includes major areas of improvement and specific aims to be met to achieve satisfactory performance. If the student and/or the clinical facilitator/midwifery educator/academic liaison officer have reason to believe that they cannot work together to implement the improvement plan, a request can be made by either person to the subject coordinator for alternative arrangements. Each student receives a summative assessment towards the end of her or his clinical placement, which is assessed as either overall satisfactory or unsatisfactory.
The following diagram demonstrates the process for clinical subject assessment.
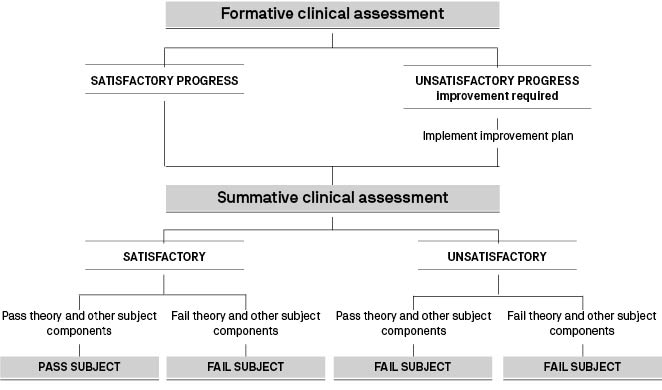
Administering of intravenous medications while on clinical practice
Third-year Bachelor of Nursing students are permitted to administer intravenous medications only under the following conditions:
- under direct supervision of a registered nurse (including University clinical supervisors) accredited by the hospital to administer intravenous medications as long as all other medication requirements have been met, e.g. correct dose, patient, route, time, and written orders, etc., and
- hospital policy allows students to administer intravenous medications under the direct supervision of a registered nurse as set out above.
